I have been chatting with many patients who are on weight loss (coupled with diabetes) medications such as Ozempic or Wegovy (AKA semaglutide). I’m happy to hear when they feel like they are getting their life back, don’t have a constant burden associated with food and body weight, have a reduction in A1C, and show improvements in blood pressure, lipid profile, and arthritic and joint pain symptoms (due to decreased weight). Like anything, there are a million shades of gray and I think it’s important to take a look at all the possible variations when stepping into a long-term drug application that may be setting you up for more risk than reward.
Remember, I’m here to be impartial and support you with long-term wellness, not judge going on weight loss medications. I think they have a clinical place, but need to be carefully scrutinized for each unique person. I want to empower each of us to make educated and discerning decisions about the one vessel we get this lifetime. Put in the time.

Long-Term Safety:
Diet drugs generally only suppress weight while a person is taking them, and many of them turn out to be unsafe for long-term use, meaning that they really aren’t a permanent “solution” for weight loss. There are a number of examples, but the most infamous one might be the diet pill fen-phen, which became wildly popular in the early 1990s and then was pulled from the market after 5 years because it was found to cause heart-valve defects.
More recently, in 2020, the FDA asked the manufacturer of another diet pill (Belviq) to withdraw it from the market, citing cancer risks. The agency had originally given Belviq the green light in 2012, making it one of only a few diet drugs to be approved for long-term use. But after further study, the FDA found that the risks posed by the drug outweighed its supposed benefits. The agency advised patients to stop taking Belviq immediately and dispose of any unused pills, and told doctors to stop prescribing and dispensing the drug.
Cases like this show how risky diet drugs can be for long-term use, risks that don’t become evident until the drugs have been studied for years. “Approving a drug for long-term use when clinical tests lasted only a year is inadequate. Drugs for depression are now being tested for five and even seven years.” The trial for Semaglutide/Wegovy lasted only a year and four months. It was also funded by the drug maker (as many early-stage pharmaceutical studies are), which is known to be a significant source of bias in research.
That makes me very nervous…how about you?

Eating Disorders and Weight Loss Medications:
You might be wondering what are the best appetite suppressants and the best over-the-counter weight loss medications. If so, that may be a sign you have disordered eating patterns. To want to dull your body’s natural signals that keep you surviving and self-caring is a call for professional help (Psychologist and Registered Dietitian). Appetite suppressants, whether they are over the counter, by prescription, natural, or chemical based, each have their own set of individual side effects. Appetite suppressants can become addictive, especially in individuals who have been diagnosed with an eating disorder, as these individuals are more likely to have compulsive and impulsive personality traits, which make them more prone to developing an addiction to substances. Substance abuse is generally thought to involve harmful drugs such as opioids, cocaine, marijuana, and alcohol. However, since appetite suppressants are stimulants, they too can be placed in the same category as “abused substances”.
Eating disorders can be complicated by substance abuse, and many treatment centers work to diagnose co-occurring conditions in individuals who are seeking treatment for their eating disorders. Co-occurring conditions are characterized by a combination of two or more mental health disorders, eating disorders, and/or substance abuse disorders.
Diet pill use in individuals with eating disorders is associated with vomiting and other purging behavior, caffeine use, novelty seeking, trait anxiety, and other Axis I and II disorders (any anxiety disorder, borderline personality disorder, or alcohol abuse or dependence). Given the observed frequency of diet pill use in individuals with eating disorders, the unregulated nature of these substances, and the ease with which they can be obtained, assessment of diet pill use (including brand, source, and dosage) should be routine.

What Happens When You Discontinue Weight Loss Medications?
To date, 3 good studies on anti-obesity medications (Belviq, Saxenda, and Wegovy) have demonstrated rapid regain once the medication has stopped. In one of these studies, it was after weight loss had been maintained for 3 years, and when the drug was discontinued the weight returned rapidly toward baseline.
Without adjacent new and consistent health behaviors like plentiful movement and wholesome eating, the weight will come back. The medication is meant to be one tool in your tool chest, but not the only tool. I have seen some great successes with patients on the new drug Wegovy or Ozempic, and some who didn’t fare well (nausea, vomiting, constipation).
Nourishing While on Weight Loss Medications
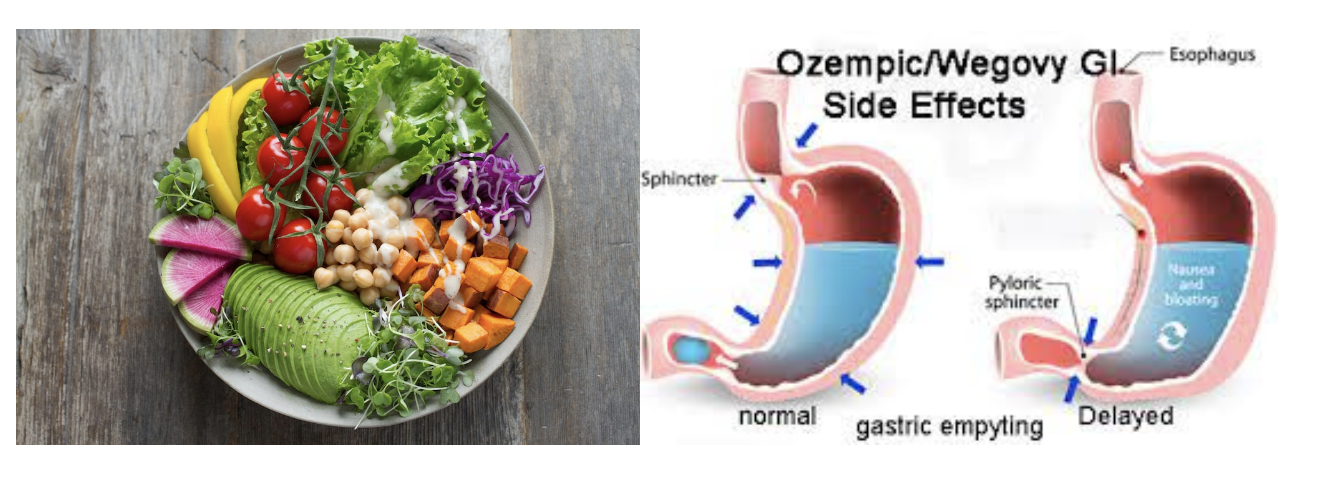
Often I have heard from patients about nausea, vomiting, and other GI symptoms that keep them from eating regular meals at consistent intervals while on Wegovy or Ozempic. And, when they do decide to eat, sometimes it’s “empty” food without nutrient density. This can lead to malnourishment even in a larger body. Immunity can decline, among many other body functions that we rely on (i.e. hormonal balance, mood stability, quality sleep, energy levels, etc).
Some questions to consider if you are weighing the pros and cons of weight loss medications:
- Have you ever been diagnosed with an eating disorder or disordered eating?
- What are your nourishment plans to keep your body fueled with essential daily nutrients on this medication?
- Do you plan to be active or are you currently?
- Do you assume you will be staying on this medication for life? If not, how will you adjust once you are off the medication?
- Are you afraid to be hungry?
- What is more of a priority for you: overall health (blood markers, vitality, etc) and well-being, or weight loss numbers and clothing size?
I would urgently ask you to speak to a clinical psychologist and registered dietitian if you are finding you are leaning towards weight loss only and have eating disorder tendencies.
Assess the long-term plan and your overall health goals, and make sure they are still in the plan if you decide to embark on the weight loss medication journey.
As a reminder, I’m not coming down on pharmaceuticals. We desperately need them! After all, I’m relying on them for cancer treatment. I am merely bringing up some thoughts that are worth exploring.
Your long-term wellness champion,
Miriam Jirari MPH, RDN, CPT, Intuitive Eating Counselor
Studio SWEAT Dietitian

Resources:
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2248697/
- https://centerfordiscovery.com/appetite-suppressants-eating-disorders/
- https://www.today.com/health/diet-fitness/weight-loss-wegovy-ozempic-rcna34709
- https://christyharrison.com/blog/the-truth-about-that-new-diet-drug
- https://www.drugs.com/medical-answers/difference-between-ozempic-wegovy-3565564/#:~:text=Official%20answer&text=Ozempic%20and%20Wegovy%20are%20the,and%20helps%20with%20weight%20loss.
- https://www.clinicalnutritioncenter.com/weightloss/weight-loss-medication/when-to-stop-weight-loss-medication
- https://www.bloomberg.com/news/features/2022-01-04/prescription-weight-loss-drugs-for-obesity-work-if-your-doctor-lets-you-get-them?leadSource=uverify%20wall
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8717485/
- https://www.rxlist.com/wegovy-side-effects-drug-center.htm
- https://www.nbcnews.com/health/health-news/new-weight-loss-drugs-effective-insurance-coverage-shortage-rcna32781









Comments - 0